Your tongue is more than just a muscle that helps you taste and articulate words. It serves as a mirror reflecting the state of both your oral environment and your overall health. Dentists often examine the tongue during routine checkups to detect subtle changes in color, texture, and moisture. These observations can unveil underlying conditions ranging from nutritional deficiencies to systemic diseases.
Anatomy of the Tongue and Its Diagnostic Value
The tongue is composed of specialized tissues, including taste buds, muscles, and a protective mucosal layer. Beneath its surface lie rich blood vessels and nerves that respond to various internal changes. A trained dentist can interpret findings such as swelling of papillae or alterations in the mucosal lining. Regular assessments of the papillae pattern help identify early signs of infections and other abnormalities.
- Fungiform papillae – Found at the tip and sides, responsible for sweet and salty tastes.
- Filiform papillae – Hair-like structures covering most of the tongue, involved in texture perception.
- Foliate papillae – Ridges on the sides, responsive to sour tastes.
- Circumvallate papillae – Large buds at the back, key for bitter taste detection.
Changes in any of these structures can raise flags about potential issues, such as oral candidiasis or glossitis. Dentists integrate tongue exams into comprehensive oral diagnostics to ensure early intervention.
Color Variations and What They Indicate
One of the most obvious clues is the tongue’s color. A healthy tongue typically appears pink with a thin white coating. Variations can point to specific concerns:
- Bright red tongue – May indicate glossitis or a deficiency in vitamins B2, B3, B6, or B12. Dentists may recommend blood tests to confirm nutritional imbalances.
- Pale or white tongue – Could signal anemia, dehydration, or heavy coating due to bacterial overgrowth. A thick white layer is often seen in xerostomia (dry mouth), which fosters microorganisms growth.
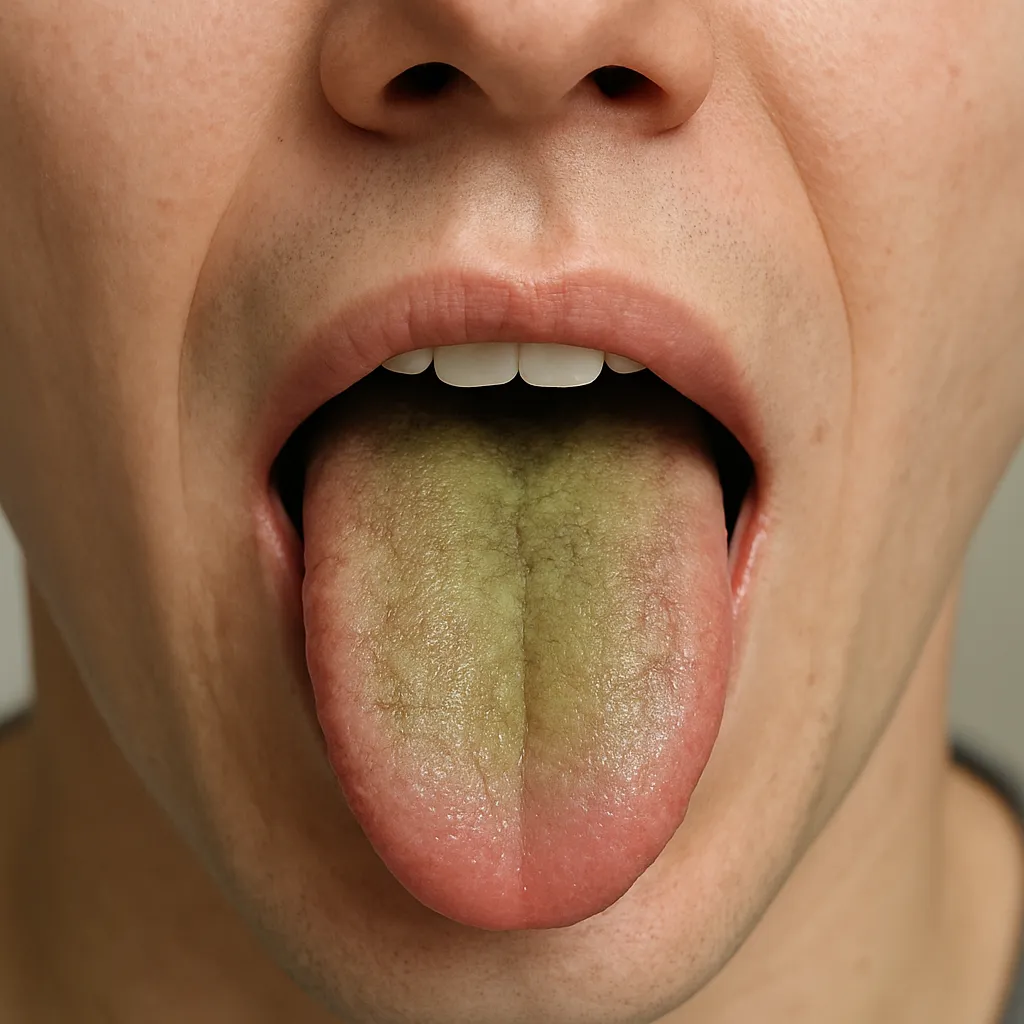
- Yellow or greenish hue – Commonly associated with bile imbalances, smoking, or poor oral hygiene that allows pigment-producing bacteria to thrive.
- Black hairy tongue – Despite its alarming name, this condition results from elongation of filiform papillae and accumulation of debris. It’s often harmless but requires improved cleaning techniques.
Identifying these color changes empowers dentists to propose targeted treatments, from nutritional counseling to antimicrobial rinses.
Texture and Surface Abnormalities
Beyond color, the tongue’s surface texture can reveal inflammation and structural changes. Dentists pay close attention to:
- Lumps or nodules – Potential signs of benign or malignant growths. Any persistent bump warrants further investigation and possible biopsy.
- Sores or ulcers – Recurrent aphthous ulcers might be linked to stress or immune system fluctuations. Persistent lesions could require referral to an oral surgeon.
- Smooth, glossy surface – Often accompanies nutritional deficiencies or atrophic glossitis. Patients lacking proper iron or folate intake may experience discomfort while eating.
- Geographic tongue – Irregular, map-like patches lacking filiform papillae. Though usually benign, it may cause sensitivity to spicy or acidic foods.
Thorough evaluation and timely identification of these anomalies contribute to better patient outcomes and may even save lives by uncovering early-stage oral cancers.
Systemic Connections Revealed by the Tongue
The interconnection between oral and systemic health is undeniable. A dentist’s tongue exam goes beyond preparing for a filling; it can hint at diabetes, autoimmune disorders, and cardiovascular issues.
- Persistent white patches (leukoplakia) may suggest chronic irritation or potential precancerous changes.
- Severe dryness and fissures on the tongue can accompany xerostomia, which itself may result from Sjögren’s syndrome or certain medications.
- A deeply cracked tongue with a red center might point to a systemic candida overgrowth, especially in immunocompromised individuals.
- Swollen, beefy-red appearance often correlates with scarlet fever or Kawasaki disease in children.
By correlating tongue observations with patient history, dentists can refer individuals for blood work or specialist consultations, ensuring a multidisciplinary approach to care.
Impact of Oral Hygiene on Tongue Health
Maintaining a healthy tongue requires diligent oral hygiene practices. Dentists recommend:
- Daily brushing of the tongue with a soft-bristled toothbrush or specialized scraper to remove debris and bacteria.
- Using antimicrobial mouthwashes to control harmful microorganisms without disrupting beneficial flora.
- Drinking plenty of water to prevent dryness and reduce plaque accumulation on the tongue’s surface.
- Replacing toothbrushes every three months to minimize reinfection from contaminated bristles.
Proper technique is crucial. Aggressive scraping can irritate the delicate mucosa, while neglecting the tongue fosters halitosis and increases the risk of oral infections.
Professional Tongue Care in the Dental Office
During routine checkups, dentists perform a systematic tongue evaluation:
- Inspection under bright light, with the tongue gently extended using sterile gauze.
- Palpation to detect submucosal lumps or tenderness indicative of underlying pathology.
- Documentation of any anomalies in the dental chart for monitoring over time.
- Recommendations for follow-up tests or referrals when systemic disease is suspected.
Continuing education ensures that dental professionals stay up to date with the latest diagnostics and treatment protocols, from laser therapy for leukoplakia to photodynamic treatment for fungal infections.
Patient Empowerment and Home Care Strategies
Educating patients about tongue health fosters proactive habits. Dentists can guide individuals to:
- Monitor their tongue’s appearance and report any unusual changes promptly.
- Incorporate nutrient-rich foods or supplements to address deficiencies detected through tongue inspection.
- Avoid irritants such as tobacco, excessive alcohol, and overly spicy foods that can exacerbate lesions.
- Practice stress-reduction techniques, since high stress levels often correlate with recurrent oral ulcers.
Empowered patients become active participants in their care, improving both oral and systemic well-being.
Conclusion
Regular tongue examinations by dental professionals play an essential role in early detection of both oral and general health issues. By understanding the nuances of color, texture, and moisture, dentists can provide tailored recommendations, referrals, and treatments. Combined with diligent home care, these measures ensure that your tongue remains a reliable indicator of optimal health.