Maintaining oral health is essential for overall wellbeing, and understanding the distinction between dental plaque and tartar forms the foundation of effective preventive care. Many patients overlook the early signs of plaque accumulation, allowing it to harden into more stubborn deposits that jeopardize gum and tooth integrity. This article explores the nature of plaque and tartar, the underlying processes that convert one into the other, and best practices for keeping your smile healthy.
Understanding Dental Plaque
Dental plaque is a sticky film that forms constantly on your teeth and along the gumline. It consists of saliva, food particles, and an abundance of oral bacteria. These microorganisms feed on sugars and starches left in the mouth, producing acids that can attack enamel and irritate gum tissue. Regular removal of plaque is crucial to prevent its progression into more serious conditions.
Composition and Formation
- Salivary proteins and glycoproteins
- Food debris, especially carbohydrates
- Microbial colonies including Streptococcus mutans
- Extracellular polymeric substance (EPS) forming a protective biofilm
Within hours of cleaning, planktonic bacteria adhere to enamel surfaces, secrete EPS, and multiply. This early biofilm matures over 24–48 hours, posing a higher risk for demineralization and gingival inflammation.
Risks Associated with Untreated Plaque
- Enamel erosion leading to cavities
- Gingivitis, characterized by redness and bleeding gums
- Halitosis (chronic bad breath)
- Progression to periodontal disease if neglected
Proper daily hygiene disrupts biofilm formation, halting acid attacks and safeguarding dentition. Failure to manage plaque heightens the chances of irreversible tissue damage over time.
From Plaque to Tartar: The Calcification Process
When plaque remains undisturbed, minerals present in saliva—predominantly calcium and phosphate—precipitate within the organic matrix. This process of mineralization transforms soft, removable plaque into hard, calcified deposits known as dental calculus, commonly referred to as tartar.
Characteristics of Tartar
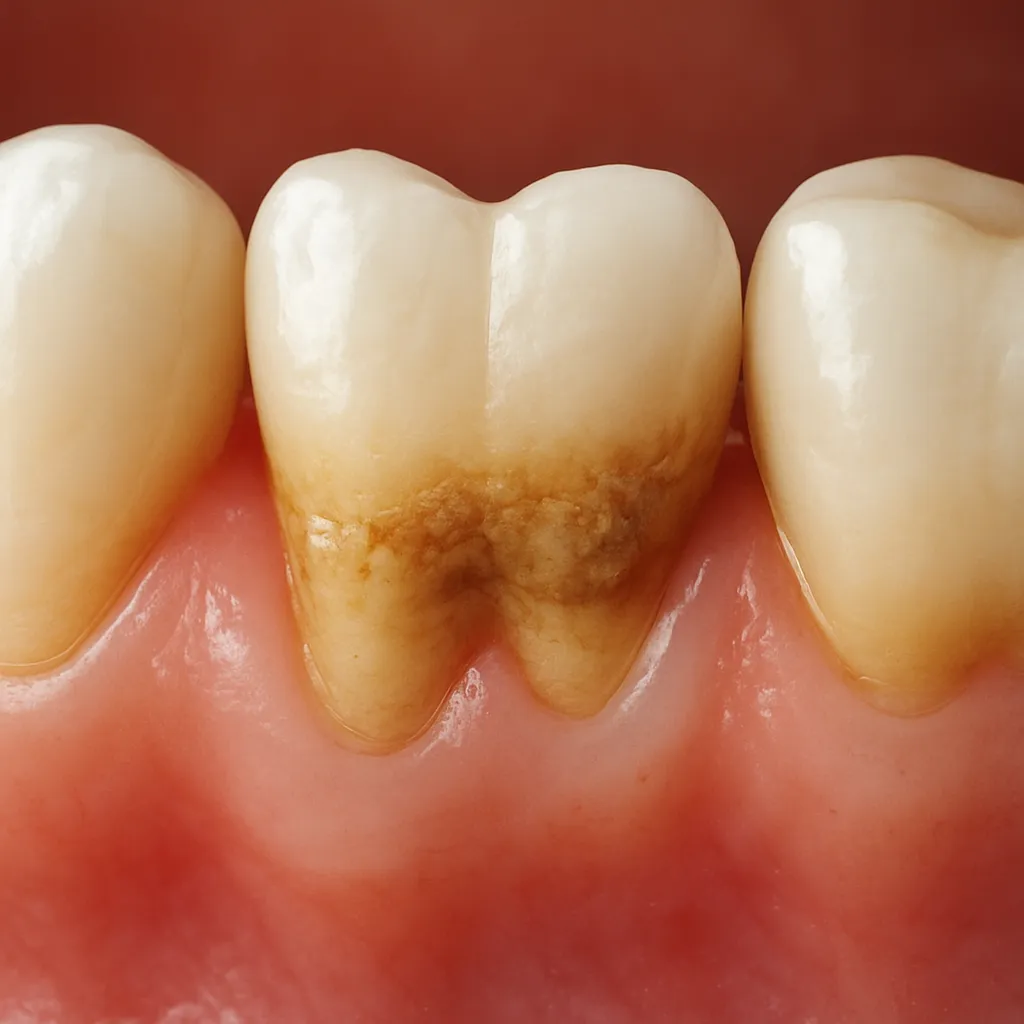
- Firm, yellow or brown crusty deposits
- Strong adhesion to tooth surfaces and subgingival areas
- Surface irregularities that harbor additional bacteria
- Difficult to remove by routine brushing and flossing
Tartar can form above (supragingival) and below (subgingival) the gumline. While supragingival calculus is visible near the gum margins, subgingival calculus often evades detection and contributes to deep periodontal pockets.
Role of Oral Hygiene Tools and Habits
Effective removal of plaque before it hardens requires consistent use of appropriate tools and techniques. Brushing alone is insufficient unless combined with interdental cleaning.
Key Practices
- Twice-daily brushing with a soft-bristled brush
- Daily brushing at a 45° angle to reach the gumline
- Interdental cleaning using floss or interdental brushes (daily flossing)
- Antimicrobial mouthrinses to target residual bacteria
Choosing a fluoride toothpaste and replacing your toothbrush every three months optimizes plaque control. Specialized electric toothbrushes may improve removal efficacy, especially in patients with limited manual dexterity.
Prevention and Treatment Strategies
Once plaque has solidified into tartar, professional intervention becomes necessary. Dentists and dental hygienists employ mechanical methods to dislodge and remove these calcified deposits, restoring a clean tooth surface and preventing further periodontal damage.
Professional Tartar Removal
- Scaling: mechanical removal of supragingival and subgingival tartar using hand instruments or ultrasonic scalers (scaling)
- Root planing: smoothing root surfaces to discourage future plaque accumulation
- Polishing: removing residual stains and creating a smooth enamel surface
Routine dental cleanings are typically recommended every six months, but patients with active periodontal disease may require more frequent visits. Early detection and removal of tartar limits bacterial colonization and supports gum reattachment.
Adjunctive Therapies
- Antibiotic gels or microspheres placed into periodontal pockets
- Chlorhexidine rinses for temporary bacterial control
- Host modulation agents to manage inflammatory response
While these treatments complement mechanical debridement, they cannot substitute for thorough prophylactic cleaning conducted by professionals.
Common Misconceptions and FAQs
Patients often confuse plaque with tartar or underestimate the importance of regular checkups. Addressing these misconceptions can improve compliance and outcomes.
Is tartar the same as plaque?
No. Plaque is a soft, sticky biofilm that can be removed by daily brushing and flossing. Once mineralized, it becomes hard tartar (calculus), which requires professional scaling to eliminate.
Can I remove tartar at home?
Home remedies and DIY tools are generally ineffective and may harm enamel or soft tissues. Only a licensed dental professional should perform tartar removal.
How often should I see a dentist for cleanings?
Most individuals benefit from dental cleanings every six months. Those with a history of rapid tartar buildup, gingivitis, or periodontitis may need more frequent appointments.
By recognizing the distinct properties of plaque and tartar, adopting meticulous oral hygiene habits, and seeking routine professional care, patients can significantly reduce the risk of cavities, gum disease, and tooth loss. Empowered with this knowledge, individuals are better equipped to preserve healthy smiles for a lifetime.