Replacing missing teeth with dental implants has become an increasingly popular option for individuals seeking a reliable and durable solution. These innovative devices not only restore function and appearance but also contribute to overall oral health by preserving bone structure. Understanding the fundamentals of implants, the procedural steps, and the care required afterward is essential for anyone considering this investment in their smile and well‐being.
Understanding Dental Implants
Definition and Components
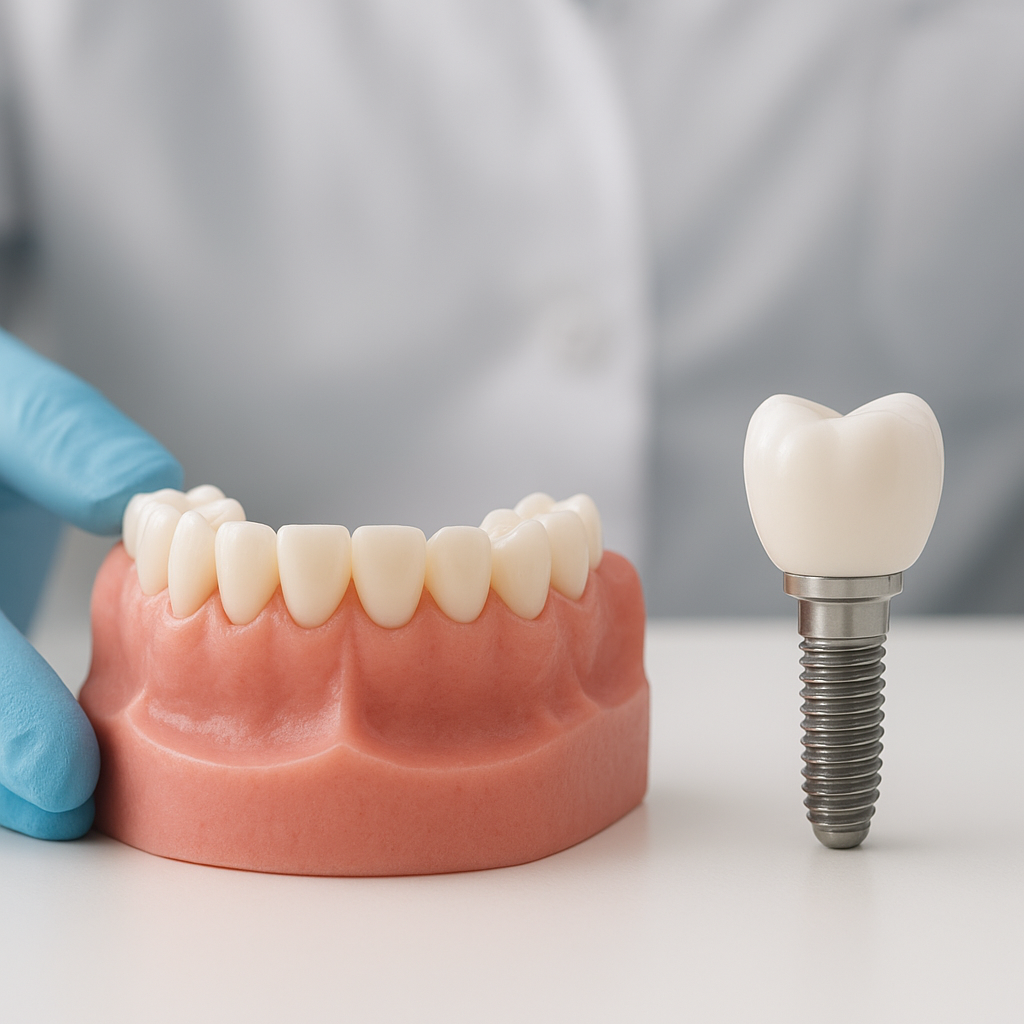
A dental implant is a small, screw‐shaped post, typically made from titanium, which is surgically placed into the jawbone to act as an artificial tooth root. Once integration occurs, a connector called an abutment is attached to support a custom‐made dental crown or bridge, referred to as the prosthesis. The three main parts of an implant restoration include:
- The implant fixture (the metallic post inserted into bone).
- The abutment (the transitional piece that links fixture to prosthesis).
- The prosthetic crown, bridge, or denture (the visible restoration).
Modern implants are engineered for biocompatibility, ensuring minimal allergic reactions and long-term stability within the bone.
Biological Process of Osseointegration
After placement, the implant undergoes osseointegration, a critical healing phase during which bone cells grow around and bond to the implant surface. This process typically extends over three to six months and establishes a robust foundation capable of resisting chewing forces. Key factors influencing successful integration include:
- Adequate bone density and volume.
- Proper surgical technique and sterile environment.
- Patient’s systemic health (e.g., control of diabetes, non‐smoking status).
When osseointegration is complete, the implant functions almost identically to a natural tooth root, providing stability and longevity to the final restoration.
The Implant Procedure: Step by Step
Initial Consultation and Planning
The journey begins with a thorough evaluation by a dental professional, often a periodontist or oral surgeon, who assesses oral structures using clinical exams and imaging techniques such as panoramic X-rays or cone-beam computed tomography (CBCT). Treatment planning may involve:
- Mapping bone height and width to determine implant size.
- Reviewing medical history and potential contraindications.
- Discussing aesthetic goals and prosthetic options (single crowns, bridges, or overdentures).
Precise planning minimizes risks and sets realistic expectations for healing time and eventual outcomes.
Surgical Procedure and Implant Placement
Under local anesthesia—or conscious sedation for anxious patients—the gum tissue is gently reflected to expose the underlying bone. A pilot hole is drilled at the predetermined site, gradually widened to match the diameter of the implant. Once the implant is securely inserted, the tissue is sutured closed, allowing for undisturbed healing. In cases of insufficient bone volume, a bone graft may be performed simultaneously or in a preparatory stage, using either autogenous bone, allografts, or synthetic substitutes.
- Surgical time typically ranges from 30 minutes to two hours, depending on complexity.
- Postoperative care includes pain management, antibiotics, and antiseptic rinses.
Patients receive detailed instructions regarding diet, hygiene, and activity restrictions to support optimal recovery.
Application of the Prosthesis
Once osseointegration is confirmed, a minor procedure exposes the implant, and the abutment is placed. Impressions are then taken to fabricate the final crown or bridge in a dental laboratory. The customized prosthesis is secured to the abutment, ensuring proper occlusion and aesthetics. Final adjustments guarantee:
- Comfortable bite alignment.
- Natural-looking contours and shade matching.
- Seamless integration with adjacent teeth and gum tissue.
Aftercare and Long‐Term Success
Oral Hygiene and Regular Check‐ups
Maintaining implants involves diligent home care and professional monitoring. Recommended practices include:
- Brushing at least twice daily with a soft‐bristle toothbrush and nonabrasive toothpaste.
- Flossing around implants using specialized implant floss or interdental brushes to remove plaque.
- Scheduling professional cleanings and examinations every three to six months.
Consistent maintenance reduces the risk of peri‐implantitis, an inflammatory condition affecting the surrounding tissues.
Identifying and Preventing Implant Failure
While success rates exceed 95% in healthy patients, implants can fail due to infection, inadequate osseointegration, or mechanical overload. Warning signs include:
- Persistent pain or discomfort at the implant site.
- Swelling, redness, or bleeding of the gum tissue around the implant.
- Mobility of the implant or prosthesis.
Early intervention can often salvage the implant. Preventive strategies encompass careful case selection, atraumatic surgical technique, and patient education on maintenance protocols.
Choosing the Right Professional and Cost Considerations
Selecting a qualified dental clinician is paramount. Look for a practitioner with advanced training in implant dentistry, such as a board‐certified periodontist or oral surgeon, and verify their portfolio of cases. A well‐equipped facility should offer digital planning tools and sterile surgical suites. Cost factors include:
- Number and type of implants required.
- Need for auxiliary procedures like bone grafts or sinus lifts.
- Type of prosthesis (fixed crown versus removable overdenture).
Although initial investment may seem significant, the long‐term benefits—in terms of function, aesthetics, and preservation of adjacent teeth—often outweigh alternative treatments. Financing plans or dental insurance coverage can make the therapy more accessible. Always seek a detailed treatment plan outlining fees, materials, and projected timelines to avoid unexpected expenses.