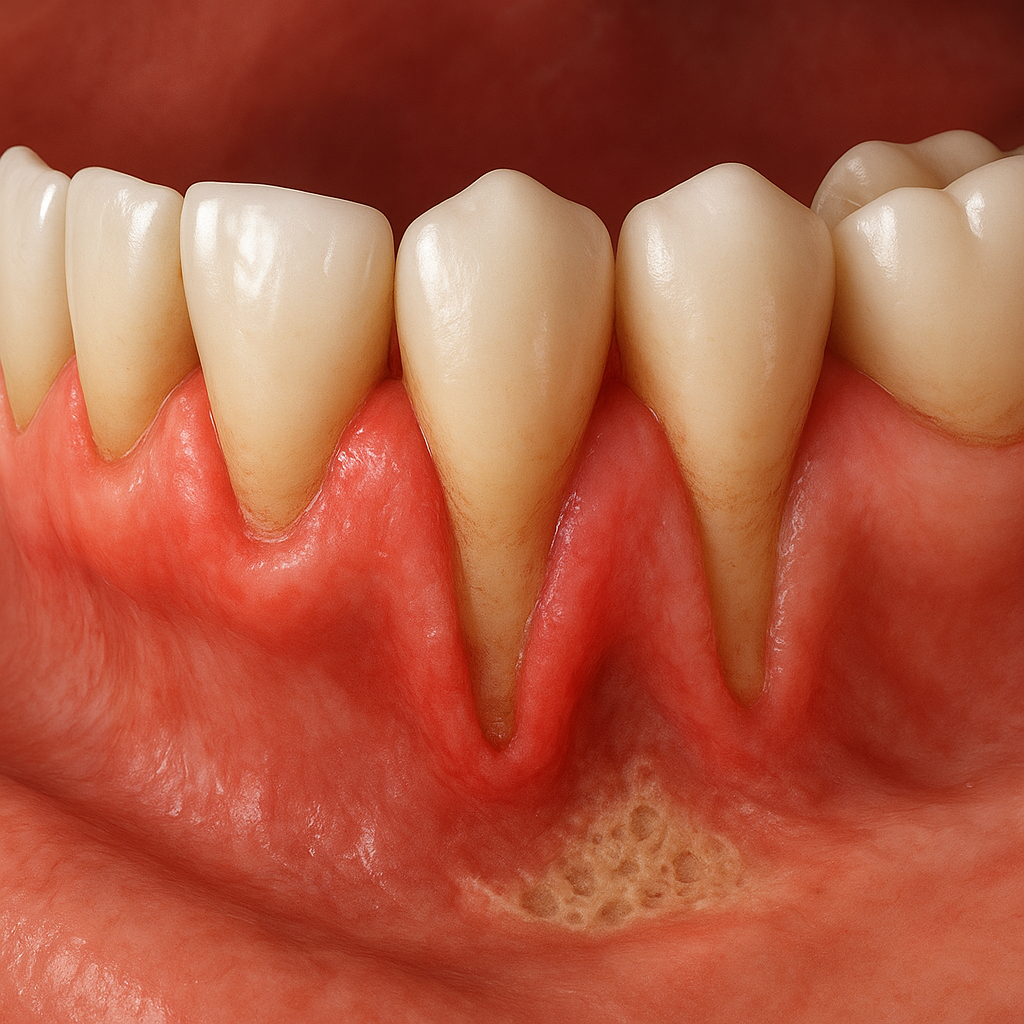
Gum recession is a common dental concern affecting millions of individuals worldwide. When the tissue surrounding the teeth gradually pulls back, exposing more of the tooth or its root, this condition can lead to increased sensitivity, aesthetic issues, and even tooth loss if left unaddressed. Understanding the underlying causes, recognizing early warning signs, and implementing effective preventive measures are essential to maintaining a healthy smile and avoiding potential complications.
Understanding the Mechanism of Receding Gums
At the core of gum recession is a complex interaction between biological factors and external insults. The gingival margin—the edge of gum tissue that surrounds and protects your teeth—can be compromised when subjected to persistent mechanical stress or chronic inflammation. The body’s immune response to bacterial invasions can inadvertently damage soft tissues, leading to the gradual loss of gum attachment.
Key elements in the recession process include:
- bacteria colonization: Dental plaque accumulates on tooth surfaces and harbor harmful microbial colonies that release toxins.
- Inflammatory response: Over time, the body’s attempt to fight off bacterial invaders leads to tissue breakdown.
- Mechanical trauma: Aggressive toothbrushing or tooth grinding exerts excessive force on gum tissue.
- Genetic predisposition: Some individuals naturally have thinner or weaker gum tissue that is more vulnerable.
Major Risk Factors for Gum Recession
While gum recession can occur for a host of reasons, certain factors significantly elevate the risk:
Poor Oral Hygiene
Inadequate brushing and flossing allow plaque to build up along the gum line. As plaque hardens into tartar, it becomes increasingly difficult to remove, which exacerbates inflammation and tissue breakdown leading to periodontal disease.
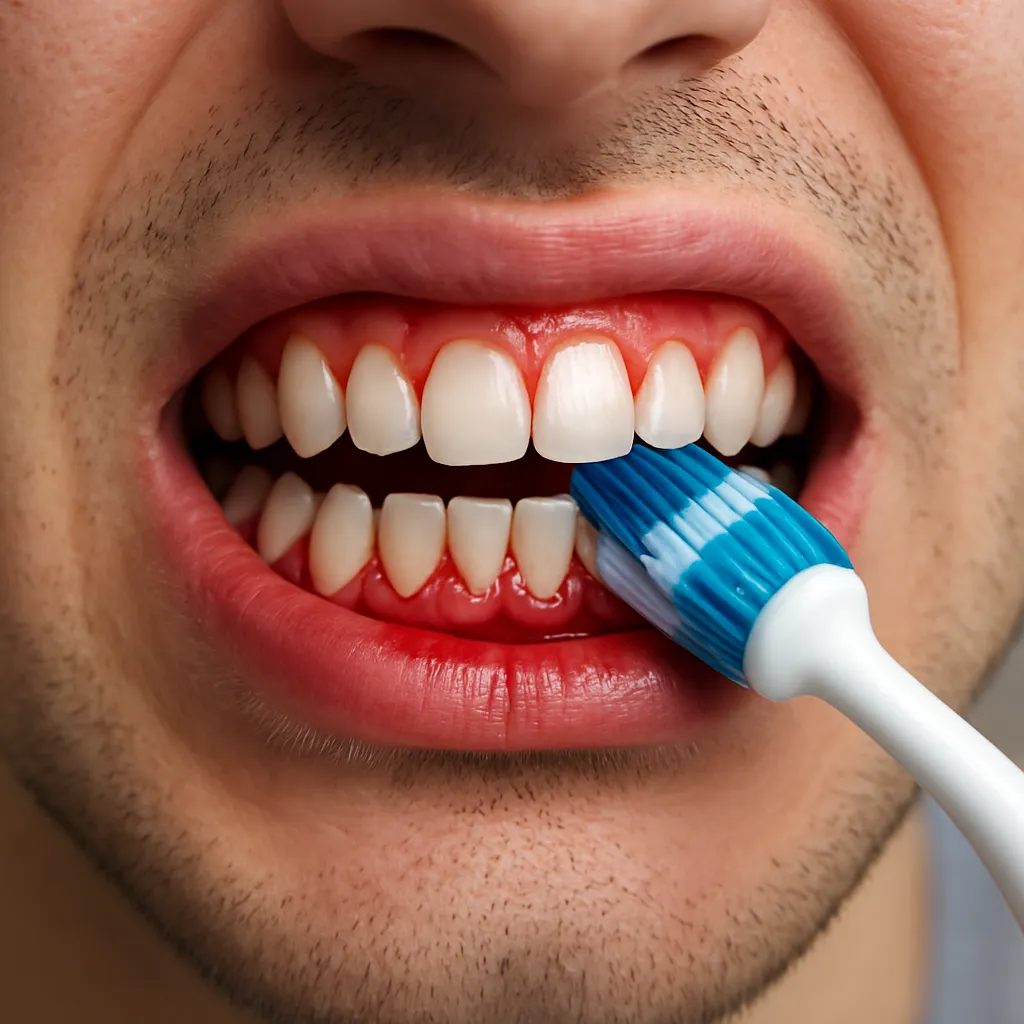
Aggressive Brushing Technique
Brushing too hard or using a hard-bristled toothbrush can erode enamel and damage soft tissue, causing mechanical trauma. Over time, this repeated force can push the gum margin backward.
Periodontal Disease
Advanced gum disease, known as periodontitis, involves deep pockets forming between teeth and gums. As the disease progresses, supporting bone and connective tissue are destroyed, resulting in noticeable gum recession.
Tobacco Use
Smoking and chewing tobacco impair blood flow to the gum tissue, reducing the body’s ability to heal and fend off infection. Smokers are up to four times more likely to develop severe gum recession.
Genetics
Certain individuals are genetically predisposed to thinner or weaker gum tissue. Those with a family history of gum disease should maintain vigilant preventive care and more frequent dental visits to identify changes early.
Hormonal Changes
Fluctuations in hormone levels—common during puberty, pregnancy, and menopause—can increase gum sensitivity and vulnerability, potentially precipitating mild recession if proper care is not maintained.
Misaligned Bite and Teeth Grinding
An uneven bite or bruxism (tooth grinding) can concentrate excessive force on specific teeth and gums, gradually wearing down protective tissues and leading to recession in targeted areas.
Recognizing Symptoms and Diagnostic Methods
Early detection of gum recession is vital. Patients often dismiss mild discomfort or sensitivity, mistaking it for routine issues like consuming hot or cold foods. However, persistent signs warrant professional evaluation.
- Tooth sensitivity: Exposed roots are less protected than enamel-covered crowns, causing sharp pain with temperature changes or acidic foods.
- Visual changes: A tooth may appear longer than its neighbors due to receding gum tissue.
- Exposed root surface: Discolored or darker areas near the gumline can indicate exposed cementum.
- Spaces between teeth: Gaps or pockets may form where gums have pulled back.
- Bleeding or swollen gums: Ongoing inflammation often accompanies the onset of recession.
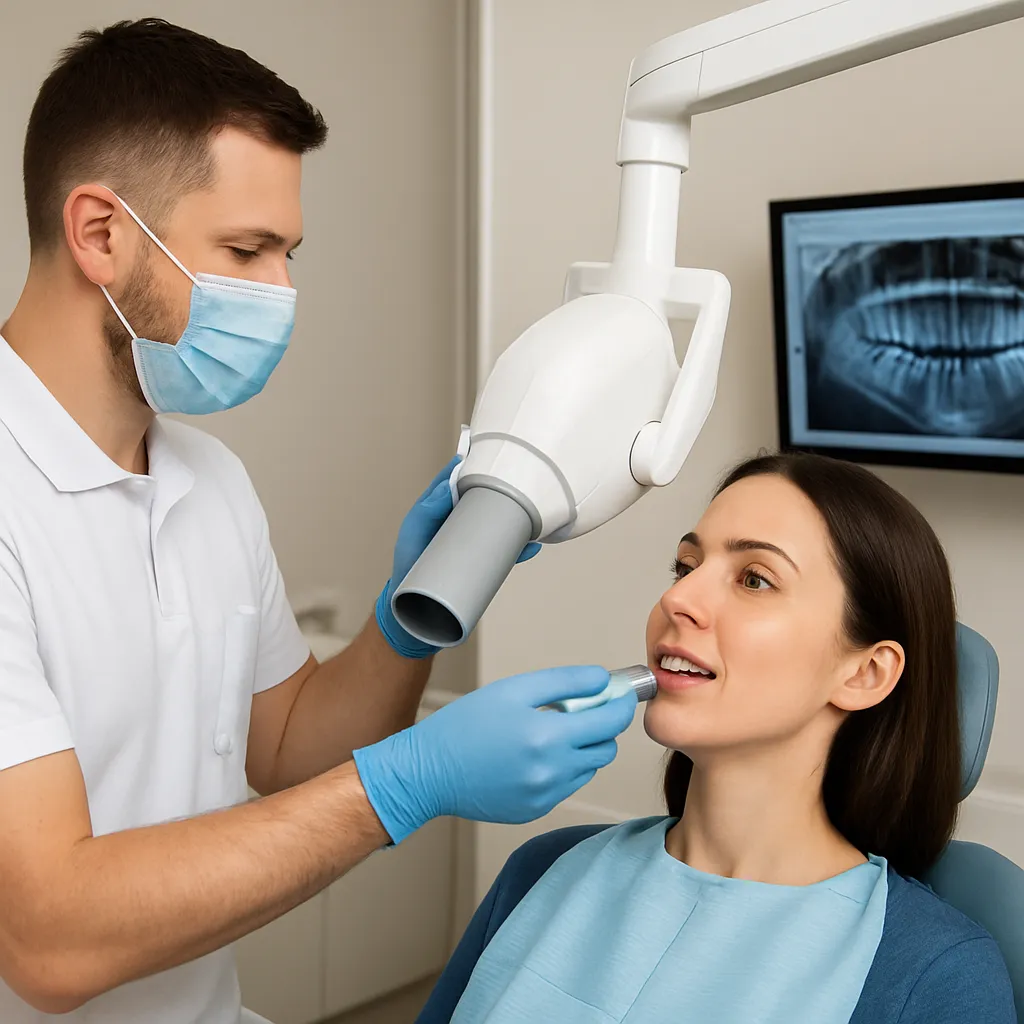
Dental professionals use a periodontal probe to measure the depth of gum pockets around each tooth. Probing depths greater than three millimeters may indicate periodontal disease. Radiographic imaging can assess bone loss, while clinical examination evaluates tissue health and mobility.
Effective Prevention Strategies
Preventing gum recession revolves around minimizing risk factors and reinforcing healthy habits. A comprehensive approach includes:
Proper Brushing Technique
Use a soft-bristled toothbrush and apply gentle, circular motions. Brushing at a 45-degree angle toward the gumline helps remove plaque without abrading tissue.
Regular Flossing and Interdental Cleaning
Daily flossing removes plaque from hard-to-reach areas between teeth. Interdental brushes or water flossers can be used as adjuncts to maintain optimal hygiene and reduce bacterial buildup.
Routine Dental Cleanings
Professional cleanings at six-month intervals—or more frequently for those with a history of gum disease—ensure thorough tartar removal and early intervention if recession is developing.
Mouthguard for Bruxism
Nightguards dissipate the excessive forces generated during teeth grinding and clenching, protecting both enamel and gum tissue from undue stress.
Smoking Cessation
Quitting tobacco not only improves overall health but also enhances gum tissue’s healing capacity and resilience.
Nutritional Support
A balanced diet rich in vitamins C and D contributes to strong collagen formation and immune defense, fortifying gum tissue against inflammation and breakdown.
Advanced Treatment Options
When preventive measures are insufficient to halt or reverse recession, dental professionals may recommend specialized treatment modalities tailored to the severity of tissue loss.
Scaling and Root Planing
Also known as deep cleaning, this non-surgical procedure involves removing plaque and tartar from beneath the gumline, followed by smoothing root surfaces to discourage bacterial colonization and promote tissue reattachment.
Antimicrobial Therapy
Local delivery of antibiotics or antimicrobial gels into periodontal pockets can reduce pathogenic bacterial counts and support healing in conjunction with mechanical debridement.
Gingival Grafting Procedures
For more significant recession, gum grafting involves transplanting tissue—often from the patient’s palate or using donor materials—to rebuild the gum margin. Common graft types include:
- Free gingival grafts
- Connective tissue grafts
- Pedicle grafts
These techniques not only cover exposed roots but also improve aesthetics and reduce sensitivity.
Guided Tissue Regeneration
This surgical approach uses barrier membranes and bone graft materials to guide the regrowth of bone and connective tissue around affected teeth, aiming to restore the natural architecture of the periodontium.
Orthodontic Correction
Misaligned teeth can exert uneven forces, promoting localized recession. Orthodontic treatment—braces or clear aligners—redistributes these forces more evenly, reducing further tissue loss and facilitating improved oral hygiene access.
Maintaining Long-Term Gum Health
Ensuring the success of both preventive and therapeutic efforts requires ongoing commitment. Patients should adhere to a personalized maintenance schedule, including:
- Consistent daily oral hygiene routines.
- Regular periodontal maintenance visits, as recommended by their dentist or periodontist.
- Monitoring for early signs of recurrence, such as increased sensitivity or new areas of recession.
- Implementing lifestyle modifications—like stress management to mitigate bruxism—and nutritional adjustments to support tissue health.
By combining vigilant home care with professional guidance, individuals can protect their gum margins, preserve the integrity of their dentition, and enjoy a more confident, comfortable smile.