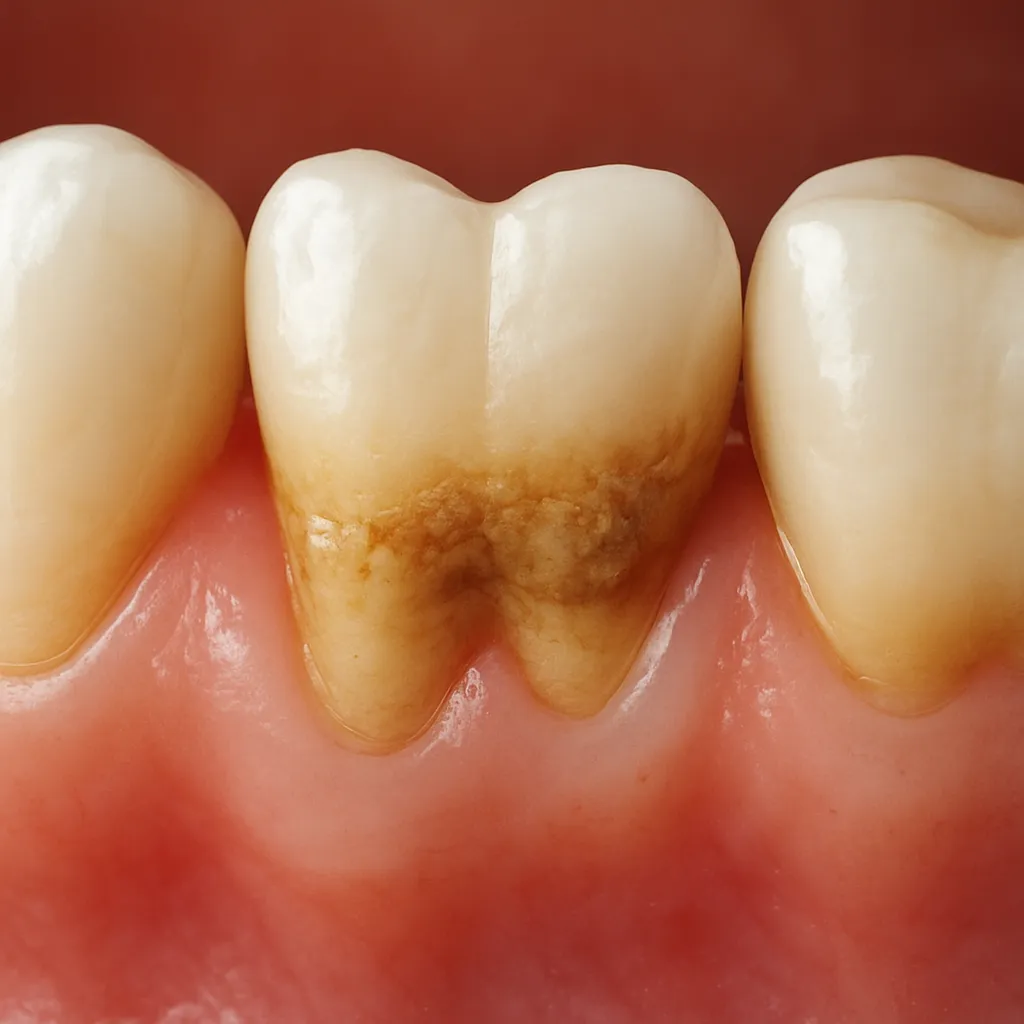
Bad breath, clinically known as halitosis, affects millions of individuals worldwide. This common condition can undermine confidence, interfere with social interactions, and signal underlying health issues. Dentists play a pivotal role in diagnosing root causes and prescribing tailored solutions. By examining the interplay of oral microorganisms, daily habits, and systemic factors, patients can overcome persistent malodor and maintain a fresh, healthy smile.
Understanding the Causes of Halitosis
Most cases of bad breath originate in the oral cavity. A complex ecosystem of bacteria thrives in hard-to-reach areas, breaking down food particles and proteins. This microbial activity produces volatile sulfur compounds (VSCs), which emit foul odors. Key contributors include:
- bacteria: Anaerobic bacteria flourish in low-oxygen environments, such as periodontal pockets and deep fissures on teeth. They release hydrogen sulfide and methyl mercaptan, potent odor-causing compounds.
- Food debris: Residual proteins trapped between teeth or on the tongue surface serve as a breeding ground for bacteria.
- tongue coating: A white or yellowish layer forms on the dorsal surface of the tongue, harboring millions of odor-producing microorganisms.
- Poor prosthetic care: Dentures, bridges, and aligners that are not cleaned properly accumulate plaque and tartar, creating niches for bacterial proliferation.
Less frequently, extra-oral factors contribute to malodor. Gastrointestinal disorders, respiratory infections, kidney or liver dysfunction, and certain medications can produce detectable odors that manifest through the mouth.
Key Risk Factors and Contributing Habits
Identifying lifestyle and health-related risk factors is crucial for a comprehensive treatment plan. The following elements often exacerbate halitosis:
- dry mouth (xerostomia): Reduced saliva production diminishes the natural cleansing action and buffering capacity of the oral environment. Medications, autoimmune diseases like Sjögren’s syndrome, and aging can all reduce salivary flow.
- saliva flow impairment: Without adequate moisture, food particles linger longer, and bacteria multiply unchecked.
- diet: Foods rich in sulfur compounds—such as garlic, onions, and certain spices—can lead to transient bad breath. High-protein, low-carbohydrate diets may also cause ketosis, releasing acetone-like odors.
- Tobacco use: Smoking and chewing tobacco introduce chemicals that irritate oral tissues, reduce taste sensation, and encourage bacterial growth.
- Alcohol consumption: Alcoholic drinks dehydrate mucous membranes and can leave a pungent aftertaste.
- Poor hygiene routines: Infrequent brushing, flossing, and neglecting tongue cleaning allow plaque and debris to accumulate.
- Systemic conditions: Chronic sinusitis, tonsillitis, and diabetes can manifest through malodor due to persistent inflammation or metabolic byproducts.
Understanding these risk factors empowers patients to adopt healthier practices and seek timely professional evaluation.
Best Practices for Daily Prevention
A robust home care regimen remains the first line of defense against persistent malodor. Dentists should emphasize the following evidence-based strategies:
- Brushing techniques: Use a soft-bristled brush to clean all tooth surfaces for at least two minutes twice daily. Angled strokes at the gumline help disrupt and remove accumulated plaque.
- Flossing: Daily interdental cleaning dislodges trapped food remnants and bacterial biofilm between teeth.
- Tongue cleaning: Employ a tongue scraper or toothbrush to gently remove the tongue coating. Target the back third of the tongue, where bacterial load is highest.
- Mouthrinses: Antibacterial rinses containing chlorhexidine, cetylpyridinium chloride, or essential oils can reduce VSC levels. Non-alcoholic formulas help maintain moisture.
- Hydration: Drinking water throughout the day stimulates saliva production and washes away residual debris.
- Chewing gum or lozenges: Sugar-free products with xylitol can enhance salivary flow and provide a temporary masking effect.
- Diet adjustments: Encourage a balanced intake of fruits and vegetables rich in fiber to mechanically cleanse teeth and neutralize acids. Limit sulfur-heavy foods when social situations demand fresh breath.
- Regular oral hygiene check-ups: Schedule professional exams and cleanings every six months to remove stubborn deposits and monitor gum health.
Consistency with these practices not only freshens breath but also supports overall oral health.
Professional Interventions and When to Seek Help
When home care measures prove insufficient, dental professionals offer targeted treatments to address persistent or severe halitosis:
- professional cleaning: Scaling and root planing remove subgingival calculus and bacterial colonies that cause malodor. This deep cleaning restores gum attachment and reduces periodontal pockets.
- Periodontal therapy: For advanced gum disease, adjunctive treatments like localized antibiotics, laser therapy, or surgical intervention may be necessary to eradicate infection.
- Assessment of prosthetics: Dentures, crowns, and orthodontic appliances should be evaluated for proper fit and cleanliness. Ill-fitting or damaged prostheses harbor bacteria and require repair or replacement.
- Saliva substitutes and stimulants: For patients with chronic xerostomia, prescription mouthwashes, gels, and sugar-free lozenges can alleviate dryness and improve comfort.
- Systemic evaluation: Collaboration with medical colleagues helps identify non-oral sources of malodor, such as respiratory, gastrointestinal, or metabolic disorders.
- Diagnostic tools: Advanced devices measure VSC concentrations to quantify malodor and monitor treatment efficacy over time.
Timely referral to a periodontist, otolaryngologist, or gastroenterologist may be indicated if initial therapies do not yield significant improvement.
Maintaining Long-Term Freshness and Oral Health
Combating bad breath is an ongoing commitment that extends beyond isolated interventions. Patients should understand that:
- Consistency is key: Adherence to a customized oral care routine prevents bacterial regrowth and keeps malodor at bay.
- Regular monitoring: Periodic reassessment of halitosis triggers allows for adjustments in therapy and lifestyle habits.
- Education: Empowering patients with knowledge about the microbial and mechanical factors behind bad breath fosters a proactive mindset.
- Interprofessional approach: Coordinating care with nutritionists, primary care providers, and specialists ensures comprehensive management of contributing conditions.
By integrating daily diligence with professional support, patients can achieve enduring confidence in their breath and overall oral well-being.